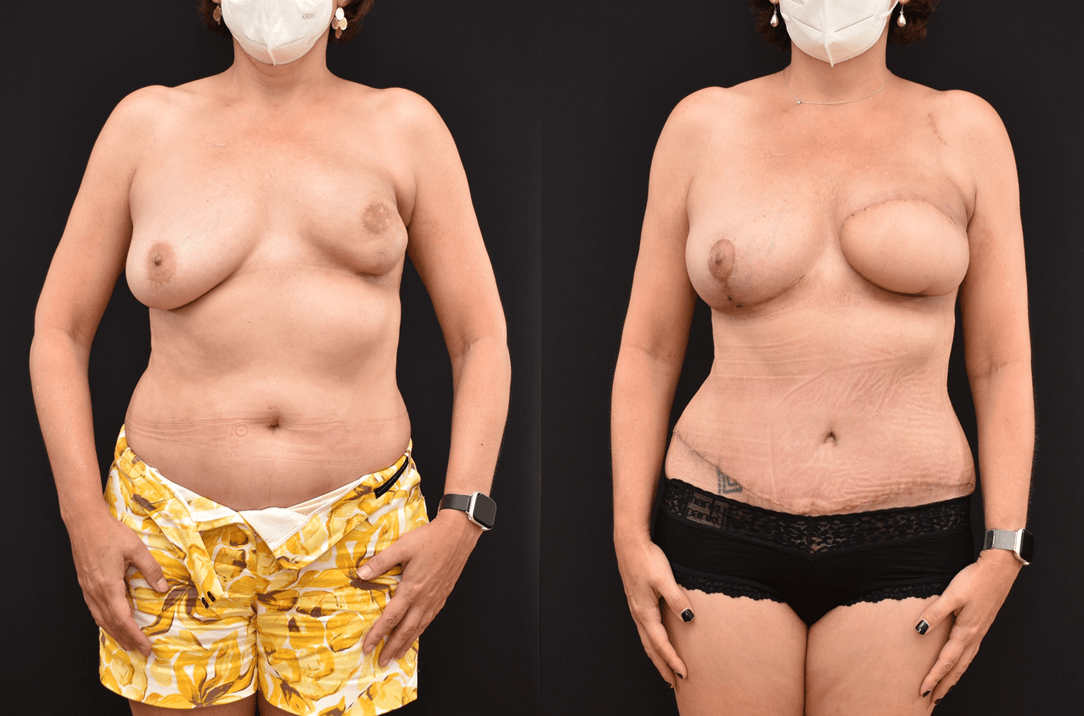
Unilateral or a single side mastectomy reconstruction can often be accomplished with a DIEP flap from the abdomen. When a unilateral mastectomy is performed it may be easier to match the non-cancer breast with skin and fat from the abdomen. This may be even more appropriate when the mastectomy has undergone radiation therapy. The radiated breast skin and tissue expander or implant can often develop a capsular contracture. Attempting to place an implant beneath a tight and constricted skin pocket can leave large disparities between the inframammary folds. This will often result in a disparity between the position of the two nipple areola complexes.
If the non-cancer breast is ptotic, or droopy, it is helpful to perform a mastopexy or lift of the breast so that the nipple areola complex, the breast, and possibly the inframammary fold can be placed in a higher position.
The radiated mastectomy skin is then removed to lower the inframammary fold on the radiated side. The superiorly displaced nipple areola complex is also removed. This skin and fat is then replaced with skin and flat from the abdomen. The recipient vessels used are the internal mammary vessels. When the flap to be utilized is large or if recipient vessels are small an additional vein from the armpit or from the shoulder can be used to augment the venous return of the flap. This can be helpful when larger skin paddles or flaps are used to reconstruct radiated mastectomy breast reconstructions.
The donor site on the abdomen is often closed under tension. After one year to 18 months the skin on the abdomen relaxes and the position and location of the abdominal scar relax and even out in position. Any asymmetry to the scar, scar hypertrophy, or keloid scars can be revised. This tends to leave a scar that is thinner and finer in appearance than during the first stage.
The flap reconstruction protocol is designed to reconstruct the breast in 3 stages. The first stage is to perform the flap and to maximize the flap survival. The second stage is performed at one to two years after the first stage and involves a procedure to improve the symmetry between the non-cancer breast and the flap reconstruction as well as to revise the abdominal donor site. The last stage is to perform a nipple areola complex reconstruction or 3-D tattoo of the nipple areola complex.
Breast reconstruction can be a rewarding aspect of a Plastic & Reconstructive surgeon’s practice.