As I continue to learn about both aesthetic and reconstructive breast surgery, I find that the same tools, skill sets, and planning that I use for aesthetic breast procedures apply to reconstructive breast surgery and vice versa.
Frequently, I see women in consultation who have undergone first a breast augmentation, second a breast reduction, and often present desiring further reduction of their breasts or require surgery for capsular contracture.
I enjoy these challenging cases as it is important to be knowledgeable of the blood supply of the nipple areola complex, the prior surgeries, and how to most effectively manage the capsular contracture.
Women who present after numerous operations often have thinning skin or breast tissue, asymmetry, capsular contracture, or unwanted motion of the implant, and desire correction.
I have found that the breast surgery techniques taught to me by Neal Handel, M.D. have been very effective for identifying, addressing, and managing these difficult cases. Capsular contracture can be very painful for the patient and interfere with daily activities and be psychologically distressing.
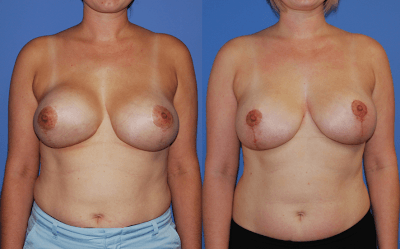
The patient in the above photograph is happy with her removal of her saline implants in exchange for silicone implants, change of implant plane, nipple areola reduction, and mastopexy. The scars are still hyperemic in this early one month post-operative result. I routinely educate patients that scars tend to be the most indurated and red approximately one month after surgery and then soften as the collagen in the scar remodels.
I have found that as larger saline implants are removed and exchanged for smaller lighter silicone implants, it is easier for patients to exercise, return to the gym, and loose weight.

Leave a reply